NTID gets $2.6M to study language outcomes
Research shows two to three out of every 1,000 children born in the United States are deaf or hard of hearing
Mark Benjamin
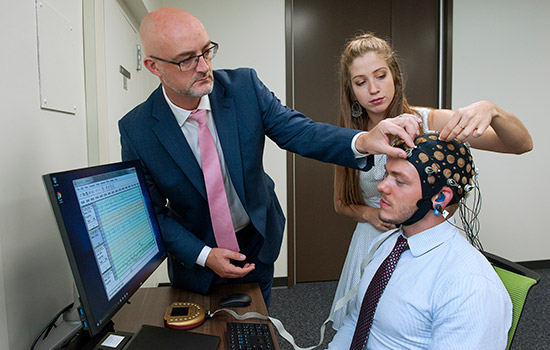
From left to right, Matthew Dye, assistant professor, director of RIT/NTID’s Deaf x Laboratory and principal investigator on the grant; Brennan Terhune-Cotter, research program coordinator in the Deaf x Laboratory; and Sarah Kimbley, student researcher.
Rochester Institute of Technology’s National Technical Institute for the Deaf has received a $2.6 million, five-year award from the National Institutes of Health’s National Institute on Deafness and Other Communication Disorders (NIDCD) to study the neurological, linguistic and behavioral outcomes for deaf individuals after childhood. It is the first study of its kind with college-age adults.
According to the latest data from the NIDCD, two to three out of every 1,000 children born in the United States are deaf or hard of hearing. For some of these children, being deaf can preclude typical acquisition of spoken language.
Some children use hearing aids, some learn sign language only, spoken language only, or a combination of sign and spoken language, with or without hearing aids. Still others use a cochlear implant, an electronic medical device that replaces the function of the inner ear and can provide sound signals to the brain. Children with a cochlear implant may use sign language, spoken language or both. As of 2012, around 38,000 children in the United States had received a cochlear implant.
“For many of these children, a cochlear implant has permitted access to spoken language,” said Matthew Dye, an RIT/NTID researcher who is leading the grant. “However, what is perhaps most striking about spoken language outcomes following cochlear implantation is the variability.”
According to the National Center for Biotechnology Information, there is wide variation in individual outcomes following cochlear implantation, and some cochlear implant recipients never develop usable speech and oral-language skills. The causes of this variation in outcomes are only partly understood at the present time.
“Understanding this variability is the first step in developing effective interventions to move a greater number of children toward better communication outcomes,” Dye said.
The research will be one of the first large-scale studies to examine spoken language outcomes in young deaf adults who received their implants in childhood and now are enrolled at RIT/NTID. The majority of these students will vary in terms of whether or not they use their cochlear implant, the age at which they received their cochlear implant and their primary mode of communication (spoken English, sign language or other). The unique sample of young adults at RIT/NTID, many of whom learned sign language in infancy and use a cochlear implant, affords the possibility of examining how early exposure to American Sign Language (ASL) influences spoken language outcomes.
Dye will collaborate with researchers at the University of Colorado at Boulder to establish norms for hearing college students.
“The overall aim of this project is to examine the effects of auditory development, cognitive function and multimodal language outcomes in a large group of young deaf adults,” Dye said. “The results of this study will provide much-needed and timely answers regarding the possible benefits of early cochlear implantation and early intervention with sign language that parents and policy makers seek as they determine how best to intervene with the next generation of deaf infants who are cochlear implant recipients or candidates.”