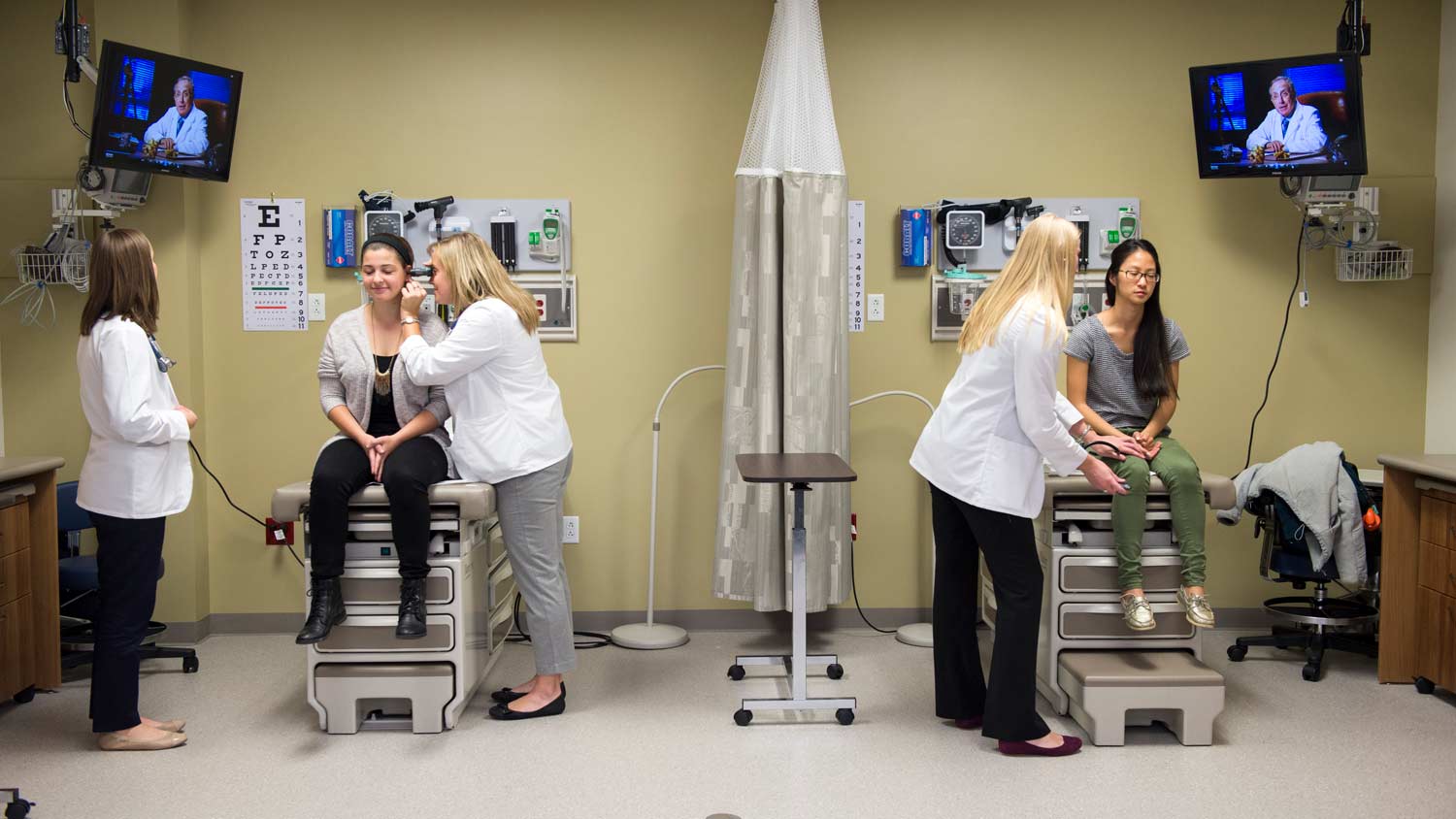
Physician Assistant BS/M Bachelor of Science Degree
Physician Assistant
Bachelor of Science/Master of Science
(BS/MS) Degree
- RIT /
- Rochester Institute of Technology /
- Academics /
- Physician Assistant BS/MS
Overview for Physician Assistant BS/MS
RIT's physician assistant program is a five-year, dual degree program where you'll earn both your bachelor's and your master's degrees.
Top five practice areas for RIT physician assistants include 1) surgical subspecialty, 2) emergency medicine, 3) internal medicine–general, 4) hospital medicine, and 5) general surgery.
88% five-year, first-time exam taker pass rate on the Physician Assistant National Certifying Examination® (PANCE).
Mandatory medical rotations in pediatrics, internal medicine, women's health, emergency medicine, surgery, orthopedics, behavioral health, and family medicine, and two elective rotations in an area of your choosing.
Recent physician assistant graduates are employed by Comprehensive & Interventional Pain Management LLP, Danbury Hospital, Harborview Medical Center, Mayo Clinic, Rochester Regional Health, St. Peter's Health Partners, SUNY Upstate Medical University, Unity Hospital, and University of Rochester Medical Center, to name a few.
Accelerated Bachelor’s/Master’s Available: Earn both your bachelor’s and your master’s in less time and with a cost savings, giving you a competitive advantage in your field.
RIT’s physician assistant program prepares you to elicit medical histories, conduct physical examinations, order laboratory and radiological testing, diagnose common illnesses, determine treatment, provide medical advice, counsel and educate patients, promote wellness and disease prevention, assist in surgery, and perform casting and suturing.
Physician assistant duties vary depending on the state and specialty in which they practice. In most states, including New York, physician assistants may prescribe medication. Examples of specialties include (but are not limited to): internal medicine, family medicine, emergency medicine, geriatrics, pediatrics, women’s health, behavioral health, general surgery, orthopedics, neurosurgery, and neonatology. Clinical rotations (internships) during students’ last year provide the opportunity to explore these varied disciplines.
Obtaining the skills and knowledge to practice as a physician assistant is a complex process. A carefully planned course of study has been developed to offer a balance of didactic and clinical knowledge. A significant component of the educational process is the socialization of the student to the character, performance, and role of a provider of medical care. The evaluation of the student’s adaptation to this role depends on the experienced judgment of individual faculty members. It is important to recognize that these subjective judgments may transcend or be independent of traditional paper and pencil tests and other similar objective measures of academic performance. Physician assistant education involves instruction from practicing clinicians with unpredictable schedules.
Many opportunities, in the form of evaluations, are provided for the measurement of progress by both faculty and student. In addition to a fully staffed Academic Support Center, individual instruction and tutoring may be provided in certain instances. Every effort is made to provide a complete learning environment. Even though a variety of experiences, learning situations, and tools are provided by the Program, the single greatest factor, motivation, is essentially up to the student.
Mission
RIT's physician assistant program provides a foundation of science and liberal arts; and prepares students to provide compassionate, patient-centered healthcare. The program is committed to developing the ethical values, medical knowledge, professionalism, and interpersonal communication skills essential for inter-professional, team-based, clinical practice.
Program Goals
1. COMPETENT: Ensure students develop the fundamental medical knowledge, skills and clinical reasoning to deliver high quality, evidence-based, patient-centered care.
2. COMPASSIONATE: Develop clinicians skilled in patient and inter-professional communication who practice with compassion, professionalism and integrity.
3. INCLUSIVE: Foster a culture of diversity, equity, and inclusion within the faculty, staff and students to deliver quality care to all patients.
5. MINDFUL: Mentor and support students’ holistic well-being and professional growth.
6. ENGAGED: Promote opportunities for student engagement in community service and outreach.
For more information view our Program Goals and Measures for Success.
Program Learning Outcomes
Medical Knowledge: Graduates will demonstrate core medical knowledge of established and evolving biomedical and clinical sciences and apply this knowledge to patient care.
Interpersonal and Communication Skills: Graduates will demonstrate interpersonal and communication skills that result in effective information exchange with patients, families, physicians, and other members of the healthcare team.
Patient Care: Graduates will provide effective, safe, high-quality, and equitable patient care in diverse settings and across the life span.
Professionalism: Graduates will practice with integrity, ethical and legal responsibility, and sensitivity to diverse patient populations.
Practice-based Learning and Improvement: Graduates will critically analyze their practice experiences with Evidence-Based Medicine (EBM) and quality assurance processes to improve patient care.
Systems-based Practice: Graduates will demonstrate awareness of and responsiveness to healthcare systems while keeping the patient at the center of cost-effective, safe care.
Learning outcomes adapted from the Competencies for the Physician Assistant Profession, written by the AAPA, ARC-PA, PAEA, and NCCPA, 2012.
Philosophy: The educational philosophy of the physician assistant program is to provide all students with the necessary liberal arts and basic science foundation necessary to build solid medical knowledge and humanistic skills by which to ultimately provide high-quality patient care to future patients. The faculty views the responsibilities of role modeling and mentoring as critical to the success of assimilating students to the realities and responsibilities of medicine today. The educational philosophy incorporates the attitudes of respect for individual patients into critical decision-making through the assimilation of appropriate interpersonal skills, compassion, and respect and reverence for the position of physician assistant.
RIT's Five-Year Physician Assistant Program: Bachelor's + Master's
The physician assistant major is offered as a BS/MS degree program, which enables students to earn both a bachelor’s degree and a master’s degree in five years. The curriculum is divided into a pre-professional phase (years 1 and 2), which includes course work in the basic sciences, mathematics, general education, and liberal arts; and a professional phase, (years 3, 4, and 5), which features didactic medical education and culminates in clinical rotations in which students apply their medical knowledge in a series of rotations through various disciplines of medicine.
Technical Standards
Students in the physician assistant program must possess certain capabilities and skills, with or without reasonable accommodation. These include the intellectual ability to learn, integrate, analyze, and synthesize data. They must have a functional use, with or without accommodation, of the senses of vision, hearing, and equilibrium. Learn more about the technical standards required of a successful physician assistant major.
Graduate Competencies
The physician assistant program has outlined functions and tasks for performing a range of skills you are expected to master as a graduate of the program. Learn more about graduate competencies required of a successful physician assistant major.
Program Progression
Students are matriculated into one of the first three years, upon their acceptance into the physician assistant major. Students must complete academic requirements to progress on to the next academic year. Students must meet all program academic requirements and standards to advance from the pre-professional phase to the professional phase of the program. Once matriculated into the pre-professional phase, students are permitted to take a limited number of courses at another institution during the summer, pending program approval. It is important, however, that students take core science courses at RIT to ensure a consistent educational experience. Students are not permitted to skip class years (i.e. first to third year) once matriculated in the major.
-
Join Us for Accepted Student Open House
Visit campus on March 28 or April 11 to meet faculty, tour campus, and ask your questions.
Careers and Clinical Rotations
Typical Job Titles
| Orthopedic Physician Assistant | Family Practice Physician Assistant | Hospitalist Physician Assistant |
| Neuromedicine ICU Physician Assistant | Cardiology Physician Assistant |
Graduates work primarily in the Health Care industry.
Clinical Rotations
Clinical rotations include a five-week experience in various disciplines of medicine, providing students with the opportunity to apply the basic principles of medicine to hospital-based and ambulatory patient care settings. Students are assigned to a primary preceptor (physician/physician assistant) and are exposed to a wide variety of acute and chronic medical problems. The emphasis is on data gathering, physical examination, differential diagnosis, patient management, maintenance of medical records, performance of diagnostic and therapeutic procedures, and the provision of patient education and counseling. Mandatory rotations are in the fields of internal medicine, family medicine, orthopedics, emergency medicine, women's health, pediatrics, general surgery, and behavioral health. Students also select two elective rotations, which enables them to customize their experience according to their medical area of interest.
The clinical rotations represent the integration and combination of the didactic and clinical phases of the physician assistant program. A great deal of planning has gone into creating a learning environment that will allow the student to obtain the high-level skills required for practice as a physician assistant. The affiliates (hospitals and office-practices) are busy places offering a variety of services. It is the responsibility of the student to explore and learn as much as possible during this very important year. You will be assigned a preceptor for each rotation by the program. This will generally be a physician, physician assistant program, or nurse practitioner who is responsible for your actions and educational experience. In general, the student is expected to participate in each and every aspect of the department or office where assigned.
The physician assistant program is fortunate to have the support of the local and neighboring medical communities for providing clinical sites offering a wide array of clinical experiences. Program faculty provides rotation assignments for all students. The program cannot assure the student assignment to a clinical affiliate within the immediate Rochester area or other desired area. Several of these sites are located some distance from the RIT main campus. The physician assistant program makes every attempt to assist the student in finding suitable housing. However, ultimately the responsibility for housing, travel, and food are the student's responsibility.
Featured Work and Profiles
-
Camp Good Days Inspired an RIT Student’s Passion for Pediatric Oncology
An RIT physician assistant student was inspired by Camp Good Days, a camp for children with cancer, which shaped her passion for pediatric oncology.
Read More about Camp Good Days Inspired an RIT Student’s Passion for Pediatric Oncology -
Breaking Boundaries: RIT Grad Merges Sonography and PA Studies for Comprehensive Patient Care
Zayneb Ghazle '24 became the first student to graduate with a double major in diagnostic medical sonography (ultrasound) and the physician assistant BS/MS program.
Read More about Breaking Boundaries: RIT Grad Merges Sonography and PA Studies for Comprehensive Patient Care -
Digital Anatomy Table Revolutionizes Learning for Physician Assistant Students
The Digital Anatomy Table is a high-tech tool that provides interactive, 3D views of human anatomy, allowing physician assistant students to explore detailed virtual cadavers and to simulate clinical...
Read More about Digital Anatomy Table Revolutionizes Learning for Physician Assistant Students -
Real-World Clinical Training Gives RIT PA Student Fresh Perspective on Patient Care
RIT PA student Juliana Lutzer gained hands-on clinical experience that deepened her understanding of patient care and enhanced her practical skills beyond classroom learning.
Read More about Real-World Clinical Training Gives RIT PA Student Fresh Perspective on Patient Care -
Doubling Down on Pediatric Care: RIT Alumna Opens Second AcuteKids Center
RIT alumna Chrysa Charno opens second AcuteKids Pediatric Urgent Care location, expanding her health care services for children.
Read More about Doubling Down on Pediatric Care: RIT Alumna Opens Second AcuteKids Center -
From RIT to Bahrain: Alumna's Fulbright Award Fuels Vital Asthma Study
RIT physician assistant alumna Maria Morcos wins a Fulbright Award. She will conduct a clinical trial on asthma in Bahrain at the Royal College of Surgeons.
Read More about From RIT to Bahrain: Alumna's Fulbright Award Fuels Vital Asthma Study
Curriculum for 2025-2026 for Physician Assistant BS/MS
Current Students: See Curriculum Requirements
Admissions and Financial Aid
The physician assistant program is a highly competitive. The number of openings for all students is limited by accreditation standards.
In addition to the university’s general admission procedures, the physician assistant major requires the completion of a supplemental data packet, application, and a personal admission interview (by invitation). The program requires a personal interview prior to admission. Interviews are by invitation only. Not all applicants are extended an invitation and not all applicants who are invited to interview are accepted into the program. The interview performance is viewed as one of the most important aspects of your application to the program. Careful attention is given to ranking and interviewing first-year and transfer applicants in comparison to their peers. In addition, the program strongly encourages applicants to have participated in some degree of patient care experience and/or shadowing of physician assistants.
There are approximately 30-36 students enrolled in each class year of the program. Therefore, the number of openings for all students is limited and competitive. All prospective applicants must have a minimum cumulative GPA of 3.0 (on a 4.0 scale) to qualify for admission and must maintain a minimum GPA of 3.0 once enrolled in the program.
It also is important to note that the minimum grade point average for acceptance into the physician assistant major is 3.0 (on the basis of a 4.0 maximum) for both high school and transfer students. In order to graduate from the major, a GPA of 3.0 or better must be maintained.
Health Care Experience
While health care experience is not an absolute requirement for admission, the program faculty highly suggest that candidates volunteer in hospitals, nursing homes, hospice and/or health care facilities, as applicable. In addition, shadowing health care professionals (PAs, MDs) in clinical arenas is highly suggested as a means of observing the role of PAs and other members of the health care team in providing care to patients.
Transfer Admission
Qualified transfer students are accepted into the major, on a space available basis. Prior health care experience and/or shadowing are strongly recommended. Transcript evaluations and rendering of transfer credit are addressed at the time of admission only. Anatomy and physiology courses must be taken within the last five years prior to matriculation to be eligible for transfer. All pre-professional course work must be completed to continue on, or to be considered for entry, into the professional phase of the major. Please contact the Office of Undergraduate Admissions for information on transfer requirements.
Advanced Placement
In the pre-professional phase, advanced placement (AP) credit for general education courses is evaluated and approved by the academic advisors. AP credit for calculus, statistics, and university electives is awarded, as applicable, within the major. AP credit is not accepted for biology and chemistry as course substitutions. Advanced placement or credit for experiential learning is not awarded for courses in the professional phase of the major.
Physician Assistant Student Employment and Co-Curricular Activities
Many PA students work during the first two years of the program. Most of these students find that balancing academics, co-curricular activities, and working 8-10 hours/week is possible. Nonetheless, attention must always remain focused on the academic expectations of the PA program, which require students to maintain a minimum term and cumulative GPA of 3.0 (BS/MS degree) throughout the program. Given the rigorous program of study, students in the professional phase of the program are strongly advised meet with their academic advisor to discuss their participation in outside employment and co-curricular activities. Students in the professional phase, including clinical rotations, must ensure that employment and/or co-curricular activities do not interfere with academic preparation, performance, clinical responsibilities, and scheduling as per clinical affiliates and program requirements. Outside commitments that are not managed effectively can dramatically affect successful progression within the program and on clinical rotations. Given the rapidly changing environment in day-to-day clinical activities and responsibilities, patient cases and/or clinical responsibilities must be given paramount priority.
Service Work
PA students participating in clinical service work are responsible for ensuring that those with whom they come into contact understand their role as PA students. At no time should PA students, participating in clinical service work, represent themselves, take the responsibility of, or the place, of qualified staff. The exception is when the student is under the guidance and direction of their instructor/preceptor for that given rotation block in which students’ status must be disclosed. PA students are never to serve as substitutions for regular staff and/or health professionals.
Summary of Costs
- RIT tuition and student fees
- Refund policy for RIT tuition and student fees
- Additional physician assistant program costs and fees
Financial Aid and Scholarships
100% of all incoming first-year and transfer students receive aid.
RIT’s personalized and comprehensive financial aid program includes scholarships, grants, loans, and campus employment programs. When all these are put to work, your actual cost may be much lower than the published estimated cost of attendance.
Learn more about financial aid and scholarships
Financial Aid Changes During the Program
Financial aid will change over the course of the Physician Assistant BS/MS program. When you are enrolled as an undergraduate student, you will be billed undergraduate tuition and fee rates, and receive undergraduate financial aid. Once you advance to graduate status, your tuition, fees, and financial aid switch to graduate tuition and aid and your undergraduate financial aid will no longer apply.
Learn more about this change
Accreditation
Resources
Program Resources
Physician Assistant Organizations
- American Academy of Physician Assistants
- New York State Society of Physician Assistants
- The Rochester Regional Physician Assistant Association
- National Commission on Certification of Physician Assistants
Wallace Library Resources
- Up-to-date Online Database
- Physician Assistant InfoGuide
- Other Medical/Health Databases
- Wallace Library Catalog and Free Services
- Rash, Rashes, and The Art of Skin Diagnosis: A Self-Paced Dermatology Tutorial, a self-paced online dermatology tutorial, introduces medical students to dermatology concepts and key terms. With a focus on how to accurately diagnose a rash, this series of Web pages also integrates morphology training with the standard dermatology curriculum diagnoses.
- Access Med
- The Medical Letters
Related News
-
October 14, 2025

RIT Ambulance expands its fleet with a second rig
RIT, which has had its own emergency medical service for more than 50 years, now has a new, second ambulance available to help students, employees, visitors, even nearby community members in need.
-
June 10, 2025

Heidi Miller retires after nearly 32 years with the physician assistant program
RIT’s physician assistant program celebrated its 30th graduating class this year, and now its biggest champion, former director and founder Heidi Miller, is preparing to retire at the end of June after nearly 32 years.
-
April 8, 2025

RIT graduate programs ranked among best in nation by ‘U.S. News & World Report’ for 2025
RIT ranked 69th overall in the nation for the best graduate engineering school based on statistical indicators that measure the quality of faculty, research, and students. The programs rose four spots from last year.
Contact

- Janice Shirley
- Senior Lectuer and Program Director, Physician Assistant
- Department of Clinical Health Professions
- College of Health Sciences and Technology
- paprogram@rit.edu